
Top 10 IBS Myths Debunked

IBS isn’t one simple problem. It’s a collection of glitches in how your gut moves, feels, and communicates with your brain.
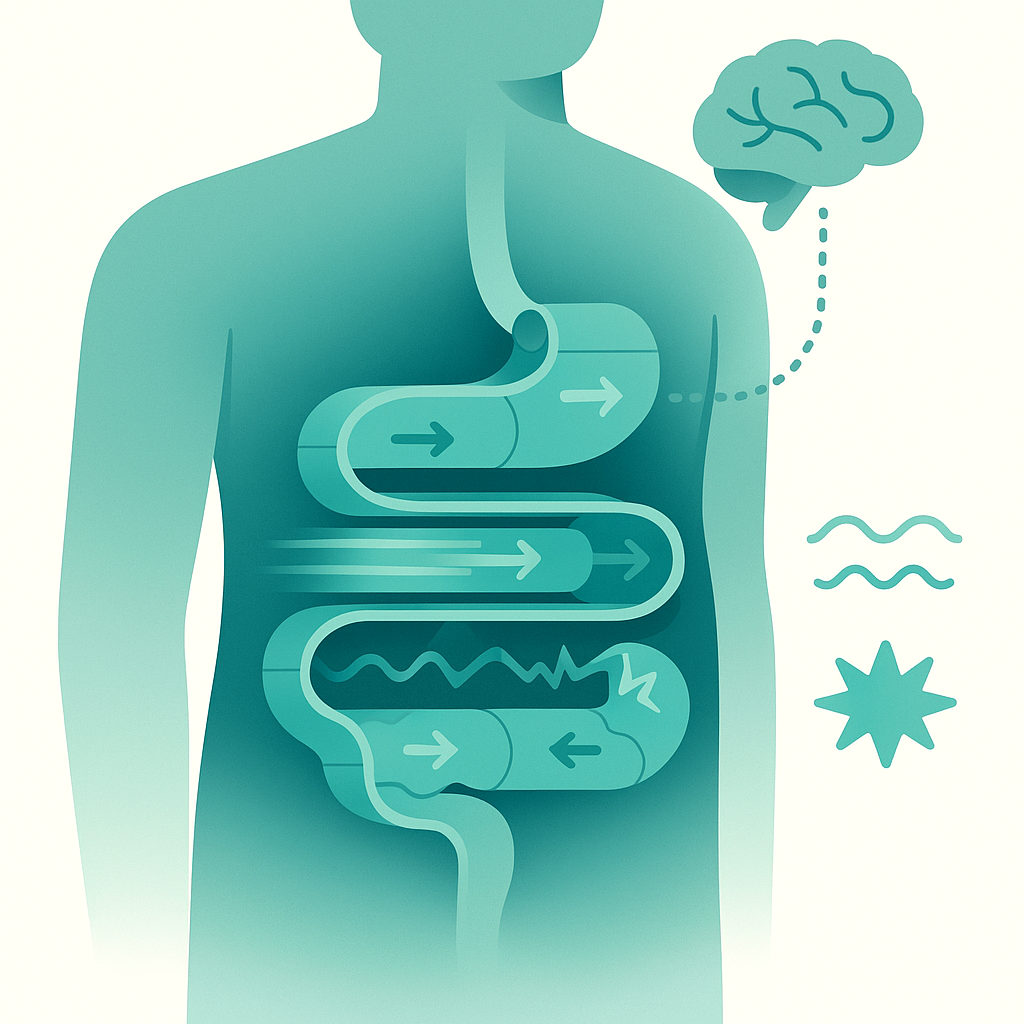
Your intestines are basically a long, muscular conveyor belt. In IBS, that belt can speed up, slow down, or spasm unpredictably. That’s motility. When it runs fast, you get urgency and loose stools. When it drags, you get constipation and that heavy, backed-up feeling.
Then there’s visceral sensitivity. Your gut is wired with nerves that send information up to your brain. In IBS, those nerves are turned up too loud. The same amount of gas that a non-IBS person barely notices can feel like a balloon in your abdomen. The gut itself isn’t “more damaged,” it’s more sensitive.
Add fermentation to the mix. Bacteria in your colon eat carbohydrates you don’t fully absorb and produce gas. That’s normal. But in IBS, gas plus altered motility plus heightened sensitivity equals pain, pressure, and bloating out of proportion to what you see on a scan.
The brain–gut axis ties it together. Your brain influences gut motility and sensitivity, and your gut sends constant updates back. It’s a noisy group chat, not a one-way street.
Clinical Reality
So how do these mechanisms turn into “my IBS is ruining my life”?
You might see patterns, even if nobody has helped you connect them. Loose mornings, backed-up evenings. Fine on vacation, miserable the week you get home. Bloating that gets worse over the day, especially after certain meals, even when the scale doesn’t move an ounce.
This is where the myths creep in. People see that stress and anxiety can flare symptoms and jump to “it’s just in your head.” That ignores the fact that your gut has its own nervous system. Of course stress changes things; it changes heart rate and blood pressure too. No one tells a person with palpitations that it’s “fake.”
Conventional advice often fails because it’s oversimplified. “Just eat more fiber” for someone who already has gas and cramps can be a disaster, especially if it’s wheat bran or a sudden big increase. “Just cut dairy and gluten” sounds decisive but skips the fact that IBS is not an allergy or an autoimmune disease like celiac.
You get pushed toward blanket diets, vague reassurance, or worse, dismissed symptoms. That’s infuriating when your daily reality is scanning for bathrooms, planning around your gut, and feeling like your body is unpredictable and slightly untrustworthy.
Practical Framework (Myth by Myth)
Instead of rapid-fire rules, think in terms of mechanisms and patterns. Here’s how to reframe the biggest myths you’ve probably heard:

Myth 1: “IBS is just stress.”
Stress is a trigger, not the cause. Your baseline wiring (motility, sensitivity, microbiome) sets the stage. Track when stress worsens things, but don’t let anyone tell you that managing stress alone is a cure.
Myth 2: “IBS causes damage to your gut.”
IBS is a functional disorder: function is off, structure is intact. No ulcers, no inflammatory destruction. That doesn’t mean it’s trivial. It means the problem is wiring and signaling, not erosion and scarring.
Myth 3: “If your tests are normal, nothing is wrong.”
Normal colonoscopies and scans just mean no structural disease like cancer or IBD. They do not rule out IBS. In fact, IBS is diagnosed after serious things are excluded and symptoms match clear criteria.
Myth 4: “More fiber helps everyone.”
Some fibers (like wheat bran) can ramp up gas and distension. Soluble fibers (like psyllium) are better tolerated, but dose and timing matter. Notice which fibers and how much your gut tolerates instead of assuming “more = better.”
Myth 5: “Cutting gluten will cure IBS.”
Gluten causes problems in celiac disease. In IBS, it’s often the FODMAP carbs in wheat (like fructans) that drive symptoms. Some people feel better when they reduce those, with or without gluten. That’s not the same as having gluten-triggered autoimmunity.
Myth 6: “If you’re bloated, you must be retaining water or gaining fat.”
Bloating in IBS is mostly gas and muscle coordination, not fluid or fat. Your abdominal wall and diaphragm can change posture during distension. That “6 months pregnant by 5pm” look can appear and disappear within hours.
Myth 7: “IBS is mild; it’s not a big deal.”
IBS doesn’t kill, but it can wreck quality of life. Work, social plans, intimacy, travel — everything gets filtered through “what if my gut acts up?” The impact is real, even if blood tests are pristine.
Myth 8: “You just need the right supplement or cleanse.”
There is no magic probiotic strain, detox tea, or parasite cleanse that fixes IBS. Some tools can help specific patterns, but anything claiming to “reset your gut in 7 days” is marketing, not medicine.
Myth 9: “All IBS is the same.”
IBS-D, IBS-C, and mixed/alternating patterns involve different motility issues and often need different strategies. A framework that helps diarrhea-predominant IBS can worsen constipation and vice versa.
Myth 10: “If changing diet doesn’t fix it, nothing will.”
Diet is one lever. Others include gut-directed medications, brain–gut therapies, and targeted movement and sleep strategies. If food changes help only partly, that doesn’t mean you’ve failed; it means another mechanism is playing a bigger role.
Use these myths as a lens when you track your symptoms. Instead of “this food is bad,” ask, “Is this pushing fermentation, sensitivity, or motility?” That’s how you move from random experiments to actual self-discovery.
CLOSING
IBS isn’t fake, it isn’t simple, and it isn’t your fault. It’s a very real brain–gut wiring problem that shows up through motility, sensitivity, and fermentation — not through dramatic lab results. Once you stop chasing myths and start understanding mechanisms, your gut stops feeling quite so mysterious. Next time, we’ll dig into how to map your personal triggers without turning every meal into a science project.